Impingement syndrome
| Impingement syndrome | |
|---|---|
| Classification and external resources | |
| Specialty | Orthopedics, sports medicine |
| ICD-10 | M75.4 |
| ICD-9-CM | 726.2 |
| eMedicine | sports/119 |
Shoulder impingement syndrome, also called subacromial impingement, painful arc syndrome, supraspinatus syndrome, swimmer's shoulder, and thrower's shoulder, is a clinical syndrome which occurs when the tendons of the rotator cuff muscles become irritated and inflamed as they pass through the subacromial space, the passage beneath the acromion. This can result in pain, weakness and loss of movement at the shoulder.[1][2]
Signs and symptoms
The most common symptoms in impingement syndrome are pain, weakness and a loss of movement at the affected shoulder.[1] The pain is often worsened by shoulder overhead movement and may occur at night, especially if the patient is lying on the affected shoulder. The onset of the pain may be acute if it is due to an injury or may be insidious if it is due to a gradual process such as an osteoarthritic spur. The pain has been described as dull rather than sharp, and lingers for long periods of a time, making it hard to fall asleep at night. [1] Other symptoms can include a grinding or popping sensation during movement of the shoulder.[3]
The range of motion at the shoulder may be limited by pain. A painful arc of movement may be present during forward elevation of the arm from 60° to 120°.[3] Passive movement at the shoulder will appear painful when a downwards force is applied at the acromion but the pain will ease once the downwards force is removed.[1]
Causes
When the arm is raised, the subacromial space (gap between the anterior edge of the acromion and the head of the humerus) narrows, through which the supraspinatus muscle tendon passes.[4] Anything that causes further narrowing has the tendency to impinge the tendon and cause an inflammatory response, resulting in impingement syndrome. This can be caused by bony structures such as subacromial spurs (bony projections from the acromion), osteoarthritic spurs on the acromioclavicular joint, and variations in the shape of the acromion. Thickening or calcification of the coracoacromial ligament can also cause impingement. Loss of function of the rotator cuff muscles, due to injury or loss of strength, may cause the humerus to move superiorly, resulting in impingement. Inflammation and subsequent thickening of the subacromial bursa may also cause impingement.[1]
Mechanism
The scapula plays an important role in shoulder impingement syndrome.[5] It is a wide, flat bone lying on the posterior thoracic wall that provides an attachment for three different groups of muscles. The intrinsic muscles of the scapula include the muscles of the rotator cuff- the subscapularis, infraspinatus, teres minor and supraspinatus .[6] These muscles attach to the surface of the scapula and are responsible for the internal and external rotation of the glenohumeral joint, along with humeral abduction. The extrinsic muscles include the biceps, triceps, and deltoid muscles and attach to the coracoid process and supraglenoid tubercle of the scapula, infraglenoid tubercle of the scapula, and spine of the scapula. These muscles are responsible for several actions of the glenohumeral joint. The third group, which is mainly responsible for stabilization and rotation of the scapula, consists of the trapezius, serratus anterior, levator scapulae, and rhomboid muscles and attach to the medial, superior, and inferior borders of the scapula. Each of these muscles has their own role in proper shoulder function and must be in balance with each other in order to avoid shoulder pathology. Abnormal scapular function is called scapular dyskinesis. One action the scapula performs during a throwing or serving motion is elevation of the acromion process in order to avoid impingement of the rotator cuff tendons.[5] If the scapula fails to properly elevate the acromion, impingement may occur during the cocking and acceleration phase of an overhead activity. The two muscles most commonly inhibited during this first part of an overhead motion are the serratus anterior and the lower trapezius.[7] These two muscles act as a force couple within the glenohumeral joint to properly elevate the acromion process, and if a muscle imbalance exists, shoulder impingement may develop.
Diagnosis
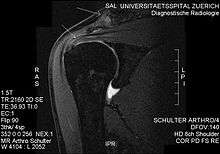
Impingement syndrome can usually be diagnosed by history and physical exam. On physical exam, the physician may twist or elevate the patient's arm to test for reproducible pain (Neer sign and Hawkins-Kennedy test). These tests help localize the pathology to the rotator cuff; however, they are not specific for impingement.[8] Neer sign may also be seen with subacromial bursitis.[9]
The physician may inject lidocaine (usually combined with a steroid) into the bursa, and if there is an improved range of motion and decrease in pain, this is considered a positive "Impingement Test". It not only supports the diagnosis for impingement syndrome, but it is also therapeutic.[10]
Plain x-rays of the shoulder can be used to detect some joint pathology and variations in the bones, including acromioclavicular arthritis, variations in the acromion, and calcification. However, x-rays do not allow visualization of soft tissue and thus hold a low diagnostic value.[1] Ultrasonography, arthrography and MRI can be used to detect rotator cuff muscle pathology. MRI is the best imaging test prior to arthroscopic surgery.[1] Due to lack of understanding of the pathoaetiology, and lack of diagnostic accuracy in the assessment process by many physicians,[11] several opinions are recommended before intervention.
Treatment
Impingement syndrome is usually treated conservatively, but sometimes it is treated with arthroscopic surgery or open surgery.[12] Conservative treatment includes rest, cessation of painful activity, and physical therapy. Physical therapy treatments would typically focus at maintaining range of movement, improving posture, strengthening shoulder muscles, and reduction of pain. Physical therapists may employ the following treatment techniques to improve pain and function: joint mobilization, interferential therapy, accupuncture, soft tissue therapy, therapeutic taping, rotator cuff strengthening, and education regarding the cause and mechanism of the condition. NSAIDs and ice packs may be used for pain relief.[3][12]
Therapeutic injections of corticosteroid and local anaesthetic may be used for persistent impingement syndrome.[12] The total number of injections is generally limited to three due to possible side effects from the corticosteroid.[3]
A number of surgical interventions are available, depending on the nature and location of the pathology. Surgery may be done arthroscopically or as open surgery. The impinging structures may be removed in surgery, and the subacromial space may be widened by resection of the distal clavicle and excision of osteophytes on the under-surface of the acromioclavicular joint.[3] Damaged rotator cuff muscles can be surgically repaired.
History
Impingement syndrome was reported in 1852.[3] Impingement of the shoulder was previously thought to be precipitated by shoulder abduction and surgical intervention focused on lateral or total acromionectomy.[3][13] In 1972, Charles Neer proposed that impingement was due to the anterior third of the acromion and the coracoacromial ligament and suggested surgery should be focused on these areas.[3][13] The role of anteriorinferior aspect of the acromion in impingement syndrome and excision of parts of the anteriorinferior acromion has become a pivotal part of the surgical treatment of the syndrome.[3]
Criticism
Subacromial impingement is not free of criticism. First, the identification of acromion type shows poor intra- and inter-observer reliability.[14][15] Second, a computerized three-dimensional study failed to support impingement by any portion of the acromion on the rotator cuff tendons in different shoulder positions.[16] Third, most partial-thickness cuff tears do not occur on bursal surface fibers, where mechanical abrasion from the acromion does occur.[17][18] Fourth, it has been suggested that bursal surface cuff tears could be responsible for subacromial spurs and not the opposite.[19][20][21][22] And finally, there is growing evidence that routine acromioplasty may not be required for successful rotator cuff repair, which would be an unexpected finding if acromial shape had a major role in generating tendon lesions.[23] In summary, despite being a popular theory, the bulk of evidence suggest that subacromial impingement probably does not play a dominant role in many cases of rotator cuff disease.[24]
See also
References
- 1 2 3 4 5 6 7 Fongemie AE, Buss DD, Rolnick SJ (February 1998). "Management of shoulder impingement syndrome and rotator cuff tears". Am Fam Physician. 57 (4): 667–74, 680–2. PMID 9490991.
- ↑ SimonMoyes.com. "What is Subacromial Impingement?".
- 1 2 3 4 5 6 7 8 9 Chen AL, Rokito AS, Zuckerman JD (April 2003). "The role of the acromioclavicular joint in impingement syndrome". Clin Sports Med. 22 (2): 343–57. doi:10.1016/S0278-5919(03)00015-2. PMID 12825535.
- ↑ NEER, C. S. (1983). Impingement lesions. Clinical orthopaedics and related research, 173, 70-77.
- 1 2 Kibler, BW. (1998). The role of the scapula in athletic shoulder function. The American Journal of Sports Medicine, 26(2), 325-337.
- ↑ Marieb, E. (2005). Anatomy & Physiology (2nd ed.). San Francisco, CA: Pearson Benjamin Cummings.
- ↑ Cools, A. , Dewitte, V. , Lanszweert, F. , Notebaert, D. , Roets, A. , et al. (2007). Rehabilitation of scapular muscle balance. The American Journal of Sports Medicine, 35(10), 1744.
- ↑ Koester MC, George MS, Kuhn JE (May 2005). "Shoulder impingement syndrome". 118 (5): 452–5. doi:10.1016/j.amjmed.2005.01.040. PMID 15866244.
- ↑ Marreez, YM; Forman, MD; Brown, SR (May 2013). "Physical examination of the shoulder joint-Part I: Supraspinatus rotator cuff muscle clinical testing". Osteopathic Family Physician. 5 (3): 128–134. doi:10.1016/j.osfp.2013.01.005.
- ↑ Oh JH, Kim SH, Kim KH, Oh CH, Gong HS (July 2010). "Modified impingement test can predict the level of pain reduction after rotator cuff repair". 38 (7): 1383–8. doi:10.1177/0363546509359071. PMID 20522833.
- ↑ Lewis JS. (Oct 17, 2008). "Rotator cuff tendinopathy / subacromial impingement syndrome: Is it time for a new method of assessment?". British Journal of sports Medicine. 43 (4): 259–64. doi:10.1136/bjsm.2008.052183. PMID 18838403.
- 1 2 3 Taheriazam A, Sadatsafavi M, Moayyeri A (2005). "Outcome predictors in nonoperative management of newly diagnosed subacromial impingement syndrome: a longitudinal study". MedGenMed. 7 (1): 63. PMC 1681371
 . PMID 16369368.
. PMID 16369368. - 1 2 Neer CS (January 1972). "Anterior acromioplasty for the chronic impingement syndrome in the shoulder: a preliminary report". J Bone Joint Surg Am. 54 (1): 41–50. PMID 5054450.
- ↑ Zuckerman JD, Kummer FJ, Cuomo F, Greller M.Interobserver reliability of acromial morphology classification: an anatomic study. J Shoulder Elbow Surg 1997; 6:286-7.
- ↑ Peh WC, Farmer TH, Totty WG. Acromial arch shape:assessment with MR imaging" Radiology 1995; 195:501-5.
- ↑ Chang EY, Moses DA, Babb JS, Schweitzer ME. Shoulder impingement: objective 3D shape analysis of acromial morphologic features" Radiology 2006; 239:497-505.
- ↑ Loehr J, Uhthoff H. The pathogenesis of degenerative rotator cuff tears. Orthopedic Trans 1987; 11:237-44.
- ↑ Ogata S, Uhthoff HK. Acromial enthesopathy and rotator cuff tear. A radiologic and histologic postmortem investigation of the coracoacromial arch. Clin Orthop Relat Res 1990; 254:39-48.
- ↑ Thompson WO, Debski RE, Boardman ND, et al. A biomechanical analysis of rotator cuff deficiency in a cadaveric model. Am J Sports Med 1996; 24:286-92
- ↑ Chambler AF, Pitsillides AA, Emery RJ. Acromial spur formation in patients with rotator cuff tears. J Shoulder Elbow Surg. 2003; 12:314-21.
- ↑ Sarkar K, Taine W, Uhthoff HK. The ultrastructure of the coracoacromial ligament in patients with chronic impingement syndrome. Clin Orthop Relat Res 1990; 254:49-54.
- ↑ Ozaki J, Fujimoto S, Nakagawa Y, et al. (1988). "Tears of the rotator cuff of the shoulder associated with pathological changes in the acromion. A study in cadavera". J Bone Joint Surg Am. 70: 1224–30.
- ↑ Pedowitz RA, Yamaguchi K, Ahmad CS, et al. (2012). "American Academy of Orthopaedic Surgeons Clinical Practice Guideline on optimizing the management of rotator cuff problems". J Bone Joint Surg Am. 94: 163–7. doi:10.2106/jbjs.k.01368.
- ↑ Arend CF. Ultrasound of the Shoulder. Master Medical Books, 2013