Intravenous pyelogram
| Intravenous pyelogram | |
|---|---|
| Intervention | |
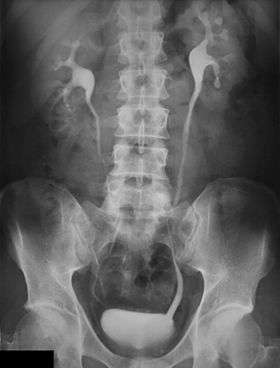 An Example of an IVU radiograph | |
| ICD-9-CM | 87.73 |
| OPS-301 code | 3-13d.0 |
An intravenous pyelogram (IVP), also called an intravenous urogram (IVU), is a radiological procedure used to visualize abnormalities of the urinary system, including the kidneys, ureters, and bladder. Unlike a kidneys, ureters, and bladder x-ray (KUB), which is a plain (that is, noncontrast) radiograph, an IVP uses contrast to highlight the urinary tract.
In IVP, the contrast agent is given intravenously, allowed to be cleared by the kidneys and excreted through the urinary tract as part of the urine. If this is contraindicated for some reason, a retrograde pyelogram, with the contrast flowing upstream, can be done instead.
Procedure
An injection of X-ray contrast medium is given to a patient via a needle or cannula into the vein, typically in the antecubital fossa of arm. The contrast is excreted or removed from the bloodstream via the kidneys, and the contrast media becomes visible on X-rays almost immediately after injection. X-rays are taken at specific time intervals to capture the contrast as it travels through the different parts of the urinary system. This gives a comprehensive view of the patient's anatomy and some information on the functioning of the renal system.
Normal appearances
Immediately after the contrast is administered, it appears on an X-ray as a 'renal blush'. This is the contrast being filtered through the cortex. At an interval of 3 minutes, the renal blush is still evident (to a lesser extent) but the calyces and renal pelvis are now visible. At 9 to 13 minutes the contrast begins to empty into the ureters and travel to the bladder which has now begun to fill. To visualize the bladder correctly, a post micturition X-ray is taken, so that the bulk of the contrast (which can mask a pathology) is emptied.
An IVP can be performed in either emergency or routine circumstances.
Emergency IVP
This procedure is carried out on patients who present to an Emergency department, usually with severe renal colic and a positive hematuria test. In this circumstance the attending physician requires to know whether a patient has a kidney stone and if it is causing any obstruction in the urinary system.
Patients with a positive find for kidney stones but with no obstruction are usually discharged with a follow-up appointment with a urologist.
Patients with a kidney stone and obstruction are usually required to stay in hospital for monitoring or further treatment.
An Emergency IVP is carried out roughly as follows:
- plain KUB or abdominal X-ray;
- an injection of contrast media, typically 50 ml;
- delayed abdominal X-ray, taken at roughly 15 minutes post injection.
If no obstruction is evident on this film a post-micturition film is taken and the patient is sent back to the Emergency department. If an obstruction is visible, a post-micturition film is still taken, but is followed up with a series of radiographs taken at a "double time" interval. For example, at 30 minutes post-injection, 1 hour, 2 hours, 4 hours, and so forth, until the obstruction is seen to resolve. This time delay can give important information to the urologist on where and how severe the obstruction is.This is very useful.
Routine IVP
This procedure is most common for patients who have unexplained microscopic or macroscopic hematuria. It is used to ascertain the presence of a tumour or similar anatomy-altering disorders. The sequence of images is roughly as follows:
- plain or Control KUB image;
- immediate X-ray of just the renal area;
- 5 minute X-ray of just the renal area.
- 15 minute X-ray of just the renal area.
At this point, compression may or may not be applied (this is contraindicated in cases of obstruction).
In pyelography, compression involves pressing on the lower abdominal area, which results in distension of the upper urinary tract.[1]
- If compression is applied: a 10 minutes post-injection X-ray of the renal area is taken, followed by a KUB on release of the compression.
- If compression is not given: a standard KUB is taken to show the ureters emptying. This may sometimes be done with the patient lying in a prone position.
- A post-micturition X-ray is taken afterwards. This is usually a coned bladder view.
Image assessment
The kidneys are assessed and compared for:
- Regular appearance, smooth outlines, size, position, equal filtration and flow.
The ureters are assessed and compared for:
- Size, a smooth regular and symmetrical appearance. A 'standing column' is suggestive of a partial obstruction.
The bladder is assessed for:
- Regular smooth appearance and complete voiding.
Contraindications
- Metformin use: Historically, the drug metformin has been required to stop 48 hours pre and post procedure, as it known to cause a reaction with the contrast agent. However the newest guidelines published by the Royal College of Radiologists suggests this is not as important for patients having <100mls of contrast, who have a normal renal function. If renal impairment is found before administration of the contrast, metformin should be stopped 48 hours before and after the procedure.[2]
- Contrast allergy: If the patient has any previous history of adverse or moderate reactions to contrast medium.[3]
Diagnoses
- Chronic pyelonephritis
- Kidney stones
- Renal cell carcinoma (RCC)
- Transitional cell carcinoma (TCC)
- Polycystic kidneys
- Anatomical variations, i.e. horseshoe kidney or a duplex collecting system
- Obstruction (commonly at the pelvic-ureteric junction or PUJ and the vesicoureteric junction or VUJ) This is very useful.
Other tests
An IVP can and should be used in conjunction with the following tests:
- Ultrasound
- Cystoscopy
- CT
- MRI
- Video cystometrography or VCMG
- Blood test
- Urine analysis
Treatment
Depending on the outcome and diagnosis following an IVP, treatment may be required for the patient. These include surgery, lithotripsy, ureteric stent insertion and radiofrequency ablation. Sometimes no treatment is necessary as stones <5mm can be passed without any intervention.
The future of the intravenous pyelogram
IVP is an affordable yet useful imaging modality and continues to be relevant in many parts of the world. In the developed world, however, it has increasingly been replaced by contrast computed tomography of the urinary tract (CT urography), which gives greater detail of anatomy and function.
However, both urography and CT urography use ionizing radiation, which involves risk to healthy tissues (potentially encouraging cancer or risking birth defects). Therefore, they are often now replaced by ultrasonography and more recently by magnetic resonance imaging (MRI), which use sound waves or magnetism instead. Also, the iodinated contrast medium used in contrast CT and contrast radiography can cause allergic reactions, including severe ones, that can be fatal in up to 1 in 25000 individuals.
Terminology
Etymologically, urography is contrast radiography of the urinary tract (uro- + -graphy), and pyelography is contrast radiography of the renal pelvis (pyelo- + -graphy), but in present-day standard medical usage, they are synonymous.
See also
References
- ↑ Page 159 in: Geoffrey D. Rubin; Mannudeep K. Kalra; Sanjay Saini (2008). MDCT: From Protocols to Practice. Berlin: Springer. ISBN 88-470-0831-X.
- ↑ Thomsen HS, Morcos SK, and members of the Contrast Media Safety Committee of the European Society of Urogenital Radiology. Contrast media and metformin. Guidelines to distinguish the risk of lactic acidosis in non-insulin dependent diabetics after administration of contrast media.European Radiology, 1999; 9: 738-740.
- ↑ Caro, J. Jaime; Evelinda Trindade; Maurice McGregor (1991). "The Risks of Death and of Severe Nonfatal Reactions with High- vs Low Osmolarity Contrast Media: A Meta-analysis". American Journal of Roentgenology. American Roentgen Ray Society. 156 (4): 825–832. doi:10.2214/ajr.156.4.1825900. PMID 1825900.
External links
| Wikimedia Commons has media related to IVP. |
- eMedicine
- NLM/MedlinePlus
- RadiologyInfo: IVP
- Cardiovascular and Interventional Radiological Society of Europe
- RCR guidlines